|
|
Home :: Skin Disorders :: Hyperhidrosis
Hyperhidrosis (Excessive Sweating) - Treatment
Alternative names :- Sweating - excessive; Perspiration - excessive; Diaphoresis
The excessive secretion of sweat from the eccrine glands, hyperhydrosis usually occurs in the axillae (typically after puberty) and on the palms and soles (often starting during infancy or childhood). Excessive sweating starts after puberty. It may be present to some degree all the time, but is at it's worst when under stress such as during exams, job interviews or dating. Excess sweating that affects areas other than the armpits and palms may a sign of serious problems.
Causes of Hyperhidrosis
Possible causes of hyperhidrosis include the following:
- Genetic factors may contribute to the development of hyperhidrosis and, in susceptible individuals, emotional stress appears to be the most common cause. Increased central nervous system (CNS) impulses may provoke excessive release of acetylcholine, producing a heightened sweat response.
- Exercise and a hot climate can cause profuse sweating in these patients
- Certain drugs, such as antipyretics, emetics, meperidine, and anticholinesterase, can increase sweating.
- In addition, hyperhidrosis may occur as a clinical manifestation of an underlying disorder. Infections and chronic diseases, such as tuberculosis, malaria, and lymphoma, may cause excessive nighttime sweating. Diabetic patients often demonstrate hyperhidrosis during a hypoglycemic crisis.
- Other predisposing conditions include pheochromocytomas; cardiovascular disorders, such as shock and heart failure; CNS disturbances (most often lesions ofthe hypothalamus); withdrawal from drugs or alcohol; menopause; and Graves' disease.
Signs and symptoms of Hyperhidrosis
The primary symptom of hydrohidrosis is wetness. However, Axillary hyperhidrosis frequently produces such extreme sweating that patients often ruin their clothes in 1 day and develop contact dermatitis from clothing dyes; similarly, hyperhidrosis of the soles can easily damage a pair of shoes.
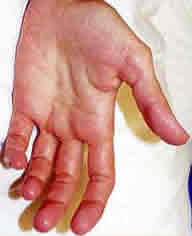
Profuse sweating from both the soles and the palms hinders the patient's ability to work and interact socially. Patients with this condition often report increased emotional strain.
Facial Hyperhidrosis, sweating of the face, may be so profuse that it causes the person to be insecure, appearing overly-anxious, when this is not really the case. Along with facial sweating, someone could experience facial blushing, another embarrassing manifestation of the activity of the sympathetic nervous system. |
 |
Diagnosis of Hyperhidrosis
Clinical observations and the patient history confirm hyperhidrosis. A number of tests may also be used to diagnose excessive sweating. Tests include:
Tests include:
- Starch-iodine test. An iodine solution is applied to the sweaty area. After it dries, starch is sprinkled on the area. The starch-iodine combination turns a dark blue color wherever there is excess sweat.
- Paper test. Special paper is placed on the affected area to absorb the sweat, then weighed. The heavier it weight, the more sweat has accumulated.
Treatment of Hyperhidrosis
The treatment of choice is the application of 20% aluminum chloride in absolute ethanol. (Most antiperspirants contain a 5% solution.) Formaldehyde may also be used but may lead to allergic contact sensitization.
Glutaraldehyde produces less contact sensitivity than formaldehyde but stains the skin; it is used more often on the feet than on the hands as a soak or applied directly several times a week and then weekly as needed. Therapy sometimes includes anticholinergics, except in patients with glaucoma or benign prostatic hyperplasia.
Severe hyperhidrosis unresponsive to conservative therapy may require local axillary removal of sweat glands or, as a last resort, a cervicothoracic or lumbar sympathectomy.
CLINICAL TIP Another form of effective treatment involves iontophoresis of water into involved areas of skin by a device that may be purchased by the patient.
Special considerations and prevention
- Provide support and reassurance because hyperhidrosis may be socially embarrassing.
- Tell the patient to apply aluminum chloride in absolute ethanol nightly to dry axillae, soles, or palms. The area should be covered with plastic wrap for 6 to 8 hours, preferably overnight, and then washed with soap and water. Repeat this procedure for several nights until profuse daytime sweating subsides.
- Frequency of treatments can then be reduced.
- Advise the patient with hyperhidrosis of the soles to wear leather sandals and white or colorfast cotton socks.
|
|





